
Our Mission
We believe no young adult (20-45yrs) should face a cancer diagnosis alone. The Whole Lotta Life Foundation is committed to providing a thriving community, support and hope for young adults in New Zealand affected by cancer.
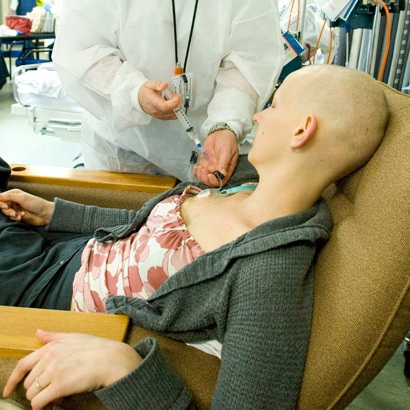
Cancer in Young Adults
While most other young adults are leading healthy, active, and busy lives, a cancer diagnosis often makes it difficult to keep up socially, academically, and professionally, as well as relate to others. It is challenging for young adults with cancer to find strong, reliable peer support as they face their illness, resulting in feelings of isolation and despair.
That's why we're here to help!




Our Programmes
We provide opportunities for our members to connect with one another, both online and in person. We are constantly working to build new programmes and channels of support.
REGIONAL MEET-UPS
We run Meet-ups in both the North and South Island. Join us for an opportunity to connect with others who get what it's like to be a young person with cancer. To see which NZ cities are holding Meet-ups this month click here
RETREAT YOURSELF GETAWAY AND WORKSHOPS
Our retreats are a great opportunity to relax, connect and enjoy some time out with other young kiwis that 'get it'. We have yoga and mindfulness classes, art therapy, outdoor adventures and lot's of time to relax and connect.
For those that can't get away for a full five days, we run one-day workshops around the country too!
CLOSED FACEBOOK GROUP
Join us online to ask questions, share concerns and connect with others. Our online group is private so you can talk openly and ask your questions without everyone on your Facebook page seeing what you've written! Click here to join

"
KAITERITERI RETREAT - 2014
For much of my cancer journey I have felt isolated. It was great to meet other young cancer thrivers, to share our stories, and forge friendships. The benefits of the retreat have continued into my life, I feel inspired to connect and support other young people who are going through cancer treatment and survivorship. I'm pretty fired up and feeling happy!"
- Laura, Breast Cancer Survivor

Get Involved
There are plenty of ways to get involved with the Whole Lotta Life Foundation whether it is as a member, a volunteer, or a donor.
Become a Member
Once you have signed up as a member you can access all of our programmes and begin connecting with other kiwis that "get it."
Volunteer opportunities
Keen to volunteer with WLL? Get in touch and let us know where your interests and talents lie, we always have room for more hands!
Make a Donation
The Whole Lotta Life Foundation relies on the donations of generous kiwis like you to keep our programmes running and growing.
